Optimize home health service logistics for better care

Home health timeliness has worsened from 2.3 days in 2019 to 3.3 days in 2024, exceeding the critical three-day target that ensures optimal patient outcomes. This decline signals deeper operational challenges affecting millions of beneficiaries nationwide. Addressing these logistics inefficiencies requires a strategic combination of AI-driven scheduling, workflow optimization, and decision support systems. Healthcare administrators can leverage technology to reduce travel time, improve visit timeliness, and enhance care coordination while maintaining cost effectiveness in an increasingly competitive landscape.
Table of Contents
- Key takeaways
- Understanding current challenges in home health service logistics
- AI and decision support: transforming scheduling and routing in home health
- Addressing nuanced operational complexities in home health logistics
- Implementing workflow optimization and outsourcing for improved outcomes
- Explore VectorCare’s patient logistics solutions
- Frequently asked questions about home health service logistics
Key Takeaways
| Point | Details |
|---|---|
| AI scheduling gains | AI driven scheduling and routing reduce travel time by 30 percent and yield 25 percent productivity gains by analyzing caregiver locations, patient addresses, skill requirements, time windows, and traffic patterns. |
| Decision support impact | Decision support systems cut travel distance by 17 percent and shrink workload deviation by 77 percent through intelligent districting and fleet management. |
| Multi objective optimization | Multi objective optimization balances cost, patient satisfaction, workload equity, and care continuity to prevent tunnel vision on a single metric. |
| Timeliness and care coordination | Technology enabled logistics improve visit timeliness, coordinate caregivers with patient preferences, and reduce missed visits across rural and urban geographies. |
Understanding current challenges in home health service logistics
Home health agencies face mounting pressure to meet timeliness benchmarks of fewer than 3 days from hospital discharge to first visit, yet performance continues declining. In 2023, 2.7 million beneficiaries received home health services with $15.7 billion in Medicare spending and 20.2% agency margins. These tight margins leave little room for operational inefficiency.
The logistics challenges extend beyond simple scheduling. Agencies must coordinate caregivers across expansive geographic territories while matching skills to patient needs, managing multiple time windows, and maintaining continuity of care relationships. Travel distances consume significant portions of caregiver time, reducing billable hours and increasing operational costs. Workload imbalances between territories create disparities in service quality and caregiver satisfaction.
Patient outcomes depend heavily on logistics execution. Delayed first visits increase readmission risks and complicate care transitions. Missed or late appointments disrupt treatment plans and erode patient trust. Geographic factors compound these challenges, with rural areas experiencing longer wait times and fewer available caregivers than urban centers. A home health scheduling app can address many of these coordination issues.
Key operational challenges include:
- Coordinating caregiver availability with patient preferences and clinical requirements
- Optimizing routes to minimize travel time while maintaining visit quality
- Balancing workloads across territories to prevent caregiver burnout
- Managing emergency visits and schedule disruptions without cascading delays
- Tracking compliance with visit frequency requirements and documentation standards
These interconnected challenges require sophisticated solutions that go beyond traditional scheduling methods. Technology platforms offer the computational power and real-time coordination capabilities needed to manage this complexity effectively.
AI and decision support: transforming scheduling and routing in home health
AI-driven scheduling and route optimization reduce travel time by 30% and achieve 25% productivity gains by analyzing multiple variables simultaneously. These systems process caregiver locations, patient addresses, skill requirements, time windows, and historical traffic patterns to generate optimal daily routes. The computational efficiency allows agencies to handle larger patient volumes without proportional increases in administrative staff.
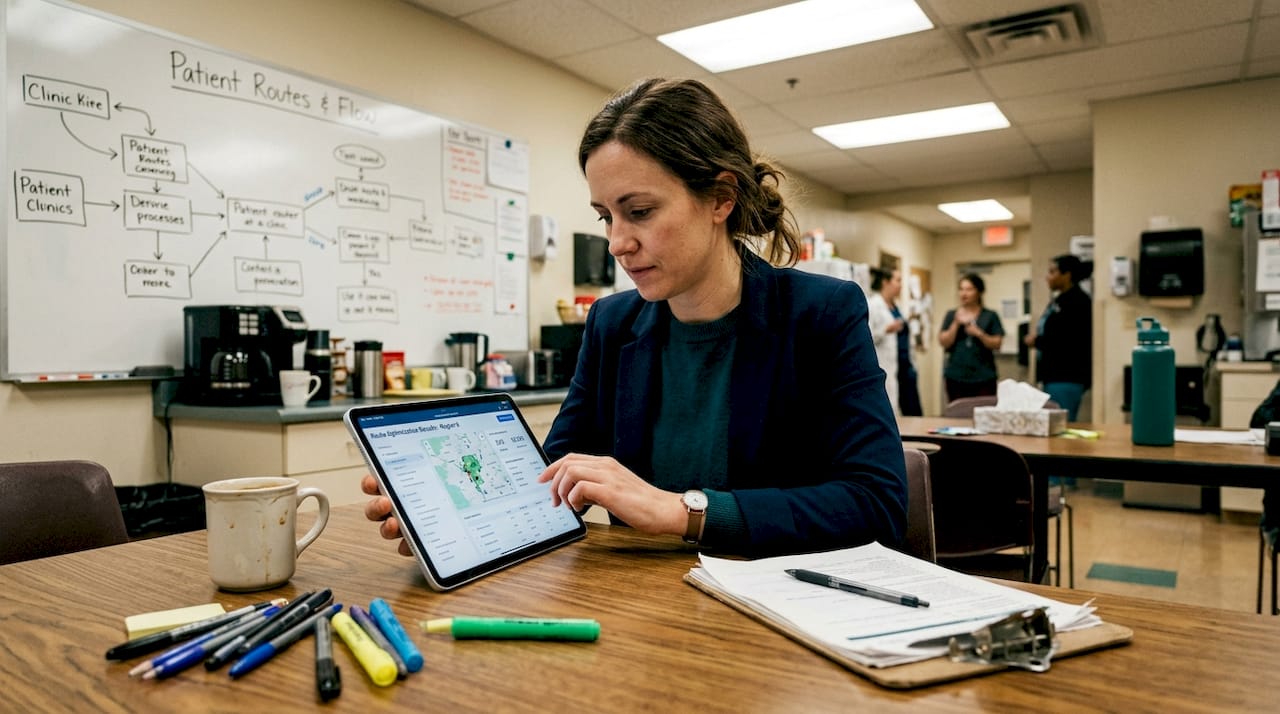
Decision support systems reduce travel distance by 17% and workload deviation by 77% through intelligent districting and fleet management. These tools analyze territory boundaries, patient density, and caregiver capacity to create balanced workload distributions. Agencies using healthcare scheduling software report fewer missed visits and improved caregiver retention.
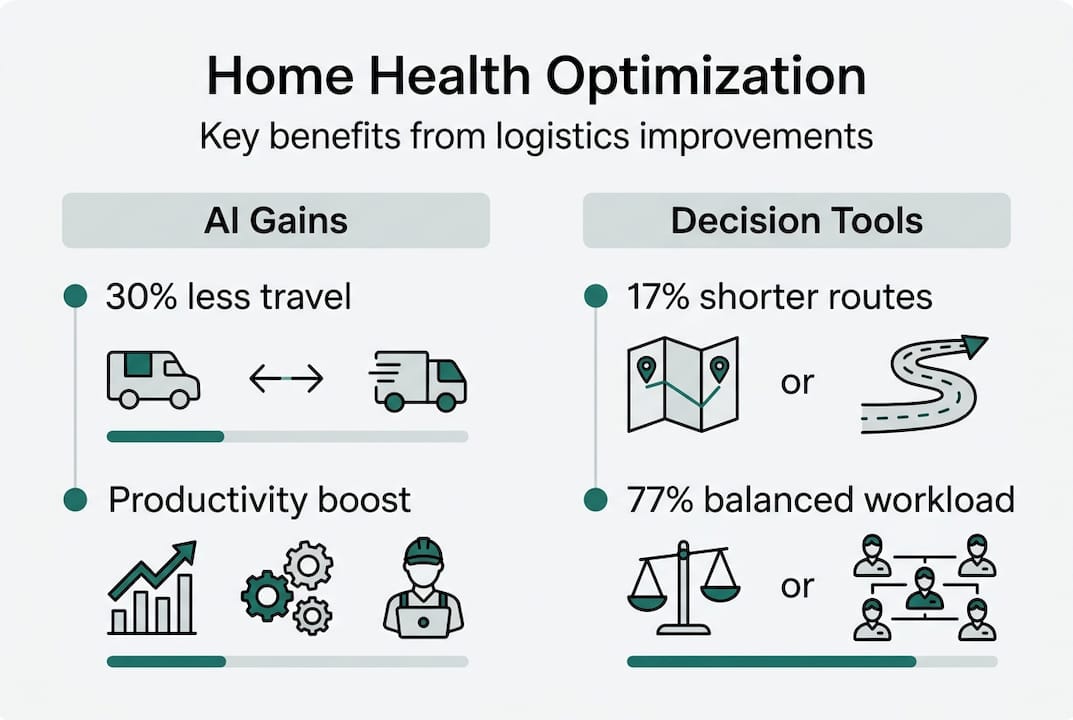
Multi-objective optimization addresses competing priorities simultaneously. Systems balance cost minimization with patient satisfaction, workload equity, and care continuity. This approach prevents the tunnel vision that occurs when optimizing for a single metric. Scheduling apps reduce missed visits by approximately 15% through automated reminders, real-time updates, and proactive rescheduling of conflicts.
| Optimization Feature | Measured Improvement | Operational Benefit |
|---|---|---|
| AI route planning | 30% travel reduction | More patient visits per day |
| Decision support districting | 77% workload balance | Reduced caregiver burnout |
| Automated scheduling | 15% fewer missed visits | Better patient outcomes |
| Predictive analytics | 25% productivity gain | Lower cost per visit |
Implementation requires integration with existing electronic health records and caregiver management systems. Agencies should prioritize platforms offering real-time updates and mobile access for field staff. Training programs help caregivers adapt to new routing patterns and communication workflows.
Pro Tip: Match caregiver skills and interpersonal compatibility when scheduling to enhance patient outcomes and reduce turnover, even if it requires slightly longer travel times.
The technology also supports growing service provider business by enabling agencies to serve more patients with existing staff. Scalability becomes possible when logistics optimization removes capacity constraints caused by inefficient routing and scheduling.
Addressing nuanced operational complexities in home health logistics
Multi-objective optimization models address skill matching, interpersonal relationships, and multiple time windows in home health logistics. These sophisticated approaches recognize that effective care coordination requires more than efficient routing. Caregiver expertise must align with patient clinical needs, from wound care and medication management to physical therapy and chronic disease monitoring.
Interpersonal relationships significantly impact care quality. Patients often prefer consistent caregivers who understand their preferences, medical history, and home environment. Models that prioritize continuity of care improve patient satisfaction and clinical outcomes, even when requiring modest increases in travel time. Balancing continuity with efficiency demands algorithms that weigh relationship value against operational costs.
Multiple time windows add complexity to scheduling optimization. Patients may require morning medication administration, afternoon wound care, and evening mobility assistance. Coordinating these windows across dozens of patients while minimizing caregiver travel requires sophisticated constraint satisfaction algorithms. Healthcare logistics solutions incorporate these constraints into optimization models.
Rural-urban disparities affect timeliness benchmarks and require tailored approaches:
- Urban agencies face traffic congestion and parking challenges but benefit from higher patient density
- Rural agencies manage longer distances between patients with fewer caregivers available
- Hybrid models combine employed and contracted caregivers to maintain coverage across territories
- Technology platforms enable coordination across dispersed teams through mobile communication and GPS tracking
“Effective home health logistics must balance multiple competing objectives including cost efficiency, patient satisfaction, caregiver workload equity, and care continuity. Single-objective optimization often creates unintended consequences in other areas.”
Hybrid fleets combining traditional vehicles with electric options represent emerging logistics themes. Sustainability considerations increasingly influence fleet decisions, particularly in urban markets where emissions regulations tighten. Route optimization software can factor vehicle range and charging station locations into planning algorithms.
Pro Tip: Prioritize flexibility in routing algorithms to handle dynamic patient needs like emergency visits or condition changes requiring immediate caregiver response.
Advanced platforms like healthcare dispatching platform solutions enable real-time adjustments to schedules based on changing conditions. This adaptability proves essential when managing the unpredictable nature of home health services.
Implementing workflow optimization and outsourcing for improved outcomes
Workflow optimization improved productivity by 10% and reduced documentation time by 5 minutes per visit in a documented case study. These efficiencies accumulate significantly over thousands of annual visits. Reducing administrative burden allows caregivers to focus on direct patient care rather than paperwork and coordination tasks.
Digital workflow tools streamline communication between field staff, coordinators, and clinical supervisors. Mobile applications enable caregivers to access patient information, document visit notes, and report issues without returning to the office. Cloud-based platforms synchronize data in real time, eliminating duplicate entry and reducing errors. Integration with billing systems accelerates reimbursement cycles.
Outsourcing logistics improved on-time shipment from 92% to 99% and achieved 12% cost savings in supply chain operations. Third-party logistics providers offer specialized expertise in inventory management, warehousing, and distribution that many home health agencies lack internally. This model works particularly well for durable medical equipment and supply kits.
Key workflow improvements include:
- Automated patient intake and eligibility verification reducing administrative time
- Mobile documentation tools eliminating paper forms and transcription errors
- Real-time schedule updates preventing miscommunication about visit changes
- Integrated billing workflows accelerating claims submission and payment
- Predictive analytics identifying patients at risk for missed visits or readmission
| Approach | In-House Management | Outsourced Logistics |
|---|---|---|
| Capital investment | High upfront costs for systems and vehicles | Lower initial investment |
| Operational control | Direct oversight of all processes | Relies on vendor performance |
| Scalability | Limited by internal capacity | Flexible scaling with demand |
| Expertise | Requires hiring specialized staff | Access to logistics specialists |
| Cost structure | Fixed costs regardless of volume | Variable costs aligned with usage |
Agencies should evaluate outsourcing for non-core logistics functions while maintaining control over clinical scheduling and patient relationships. Hybrid models combining internal care coordination with outsourced supply chain management often deliver optimal results. Strategies for reducing transportation costs apply whether managing logistics internally or through partners.
Practical implementation steps include assessing current workflow bottlenecks through time studies and caregiver feedback, selecting technology platforms that integrate with existing systems, training staff on new tools and processes with hands-on support, monitoring key performance indicators to measure improvement, and iterating based on data to refine workflows continuously.
Successful workflow optimization requires change management that addresses caregiver concerns and demonstrates tangible benefits. Involving field staff in solution selection and pilot testing increases adoption rates and identifies practical issues before full deployment.
Explore VectorCare’s patient logistics solutions
Home health agencies seeking to implement the logistics optimization strategies discussed throughout this article can benefit from purpose-built technology platforms. VectorCare offers comprehensive solutions designed specifically for patient logistics coordination, addressing the complex scheduling, routing, and workflow challenges facing modern home health operations.

The platform integrates AI-driven dispatching with real-time communication tools, enabling agencies to optimize caregiver routes while maintaining care continuity and quality. Features include automated scheduling that respects skill matching and time windows, mobile applications for field staff documentation and updates, and analytics dashboards tracking key performance metrics. Learn more about patient logistics overview and how efficiency through patient logistics transforms operations. Explore the VectorCare patient logistics platform to see how these solutions can improve your agency’s operational efficiency and patient satisfaction.
Frequently asked questions about home health service logistics
What ROI can agencies expect from logistics optimization technology?
Agencies typically see 10-25% productivity gains and 12-30% travel time reductions within six months of implementation. Cost savings from reduced mileage and increased visit capacity often recover technology investments within the first year.
How do AI scheduling systems handle emergency visits and schedule disruptions?
Advanced platforms use real-time optimization to automatically adjust routes when emergencies occur, minimizing impact on other scheduled visits. The system identifies the nearest available qualified caregiver and redistributes remaining visits to maintain coverage.
What factors matter most when matching caregivers to patients?
Clinical skill alignment, language compatibility, personality fit, and geographic proximity all influence care quality. Systems should weight these factors based on patient acuity and complexity, prioritizing clinical skills for high-need patients and continuity for stable cases.
How can rural agencies overcome geographic challenges in logistics?
Rural agencies benefit from territory clustering that groups patients geographically, hybrid staffing models combining employees and contractors, telehealth integration reducing unnecessary in-person visits, and route optimization that accounts for seasonal road conditions and longer distances.
What integration capabilities should agencies prioritize in logistics platforms?
Prioritize platforms offering bidirectional integration with electronic health records, billing systems, and caregiver management tools. Real-time data synchronization prevents duplicate entry and ensures all stakeholders access current information for coordination decisions.



